Facing COVID in a remote and resource-poor location
When I got the government order towards the end of March telling us we were to be the sole designated COVID hospital for the whole district of Simdega, I felt my heart sink.
I am the senior among three doctors in a small hospital called Shanti Bhavan Medical Centre in a village called Biru situated in the state of Jharkhand in India. I lead a team of four doctors – two senior doctors including me (I am almost 70) and two young doctors fresh out of college.
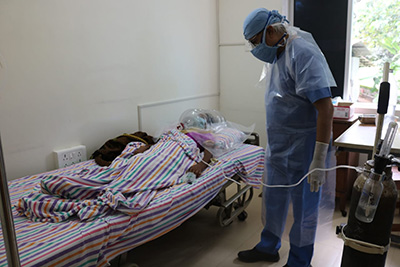
We are the only secondary-level hospital in a radius of 70-80 kilometres and for a facility like ICU there is no one else for 100 kilometres. The nearest centres that are bigger are in Ranchi and Rourkela – over 100 kilometres and a minimum of 3-4 hours of road journey away.
Surrounding the hospital are small hamlets that are predominantly inhabited by tribal people. The local people are involved in marginal farming apart from collecting forest produce. Agricultural activity goes on only during the rainy season. When there is no cultivation, the men mostly migrate to nearby states as labourers leaving behind the elderly, children and women. So, our hospital exists among a much-marginalised population.
Alcoholism is rampant among both sexes regardless of age and added to this is a high rate of illiteracy. People are so poor that often they are unable to afford even the minimum cost of treatment. This 60-bedded facility is well equipped but grossly understaffed. We deal with a wide range of emergencies like snake bites, poisoning, acute myocardial infarction and cerebral malaria. We also manage all kinds of trauma including head injury, multiple trauma and injuries due to knife attacks.
On receiving the government order, my first reaction was panic because we did not have all the resources we needed. We had not prepared any of our facilities to take care of COVID-19 patients. Then there was the worry about the safety of our staff – not just for me because I am nearing 70, but also for others who are in their 40s and 50s.
I just about managed to get protocols regarding the management of COVID-19. Being cut-off from the mainstream medical community, it was hard for us to get reliable and authentic information. Already, there was fear created in the minds of all our staff because of what was spread through social media platforms. Added to this was the impact of the nationwide lockdown with no shops, supplies or transport. It looked like we were about to walk through a dark tunnel not knowing where it would lead us.
But there was hardly any time to think as we had to ‘hit the ground running’. We had no PPE, and they were unavailable anywhere. We had no specific medicines, and our suppliers were closed. So, it was like going into a battle with no armour on our bodies and no weapons in our hands.
We used every resource to get PPE ready. There were none that could be purchased locally. Despite all these difficulties, the staff was stoic and cooperated heartily. We borrowed money and sourced whatever material we could get from local shops. Then we designed our own PPE – stitched-by-hand protective gear – with everyone pitching in. We bought bleaching powder and made hypochlorite solution and collected industrial spirit for hand sanitisers. Everything we thought necessary for treating COVID-19 patients, we improvised. We made our own four-layer cloth masks and converted plastic sheets into aprons and gumboots for protective footwear.

Then started a cascade of problems which we had not dreamed of. As a COVID hospital, we were not permitted to see any routine non-COVID patients. Thus, our main source of income vanished suddenly. Our reserves dried up and we were reduced to a hand-to-mouth daily existence, always anxious about where the next day’s means to survive would come from.
Compounding all this was the enormous social stigma attached to us being a coronavirus hospital. Many of our staff who came from nearby hamlets were prevented from coming for work because they were suspected of carrying the virus back to their neighbourhoods. They were banned from bathing in the village pond or going near any water-wells and were told not to go near the church or local shops. Many of them were threatened with violence if they persisted in coming to work at the hospital. The stigma of COVID-19 is so profound in the community that our staff were almost outcasts in their villages. The intervention by the local police did not have much effect. So, we took them all into the hospital and gave them temporary accommodation and food. This drove us deeper into debt as we had to borrow even more for supplies and food.
We prayed together every morning and evening, pleading with God to lead us. We held hands with each other promising to look after each other even if we fell ill. A conviction grew in us, slowly but surely, that we can do things with God’s help despite the seemingly insurmountable problems confronting us.
We started with whatever we had when the first patients arrived. We began with the firm trust that God was with us through this troubled journey. We felt bound to God and each other as we started taking care of the COVID-infected patients. We never failed to meet every day to pray and to uphold each other. By God’s grace we were able to source HCQ from the government supplies.
The state of Jharkhand was facing an enormous influx of migrant labourers coming back from other states and we feared that a flood of COVID-19 cases was on its way. Our fears were proven right when many among the returning labourers were found to be infected. They soon started arriving at our doorsteps – men, pregnant women and even children. They arrived exhausted, dehydrated and at times starving. Each one of them had a harrowing story about unimaginable travails on the way. They arrived with nothing but what was on their backs – not many material possessions, no money and no documents. Coming on top of all this, being infected with COVID-19 was the worst of their miseries.
What started as a trickle became a flood. At one time, we had 40 COVID+ patients in the ward including pregnant women and a three-year-old child. All of them had to be fed and cared for.
Despite all the challenges, we treated them with care and compassion without compromising the safety of the staff. We made sure they were fed nourishing food and had a restful time. It was very evident that they could not easily forget the trauma of their journey. We were most anxious about the pregnant women and the children. We were only a few doctors and nurses, but we worked around the clock despite our fears of safety and our physical exhaustion. It was a daunting task for a small community like ours.
It was difficult to convince a three-year-old child to not move out of the confines of her room. For many of them, especially the children, it must have been a frightening experience – the strict isolation and the medical workers taking care of them in strange gear with neither their faces nor their expressions clearly visible.
At one point, we thought we had reached the end of our resources and resolve. We were stretched to the limit for money, material and human power. I was not proud to be in this state and was extremely distressed to be asking staff to put their lives in danger without being able to pay them minimum wages. I had no pride left in me to even pretend that we could manage on our own. We prayed earnestly that God would find a way for us to continue walking faithfully and to serve him despite the seemingly insurmountable odds.
Then, just at the right time, many of my teachers, classmates, alumni, former colleagues and students appeared on the scene with their offers of support. Through some of these connections, many doors of generosity opened, beyond my wildest dreams.
What started as a trickle of giving soon became a stream of blessing. This brought with it gifts of money for payments of materials, PPE, medicinal supplies as well as expenses for food for all of us. These assured us of our safety and provision for our immediate needs. I could sleep easy after spending sleepless nights worrying about meeting the needs of the next day.
So far, we have treated 173 patients – both COVID+ and suspected COVID cases. All confirmed cases became negative, were discharged and sent home well. There has been no mortality. All our staff is safe, and no one has been infected as of date. All this was made possible by God’s grace as well as the goodness and support of so many connected with Christian Medical College Vellore, my alma mater.
The fight continues. But we believe that we are not alone in this far, forgotten corner of India, waging a lonely struggle against this unseen enemy. God has been with us constantly. We have survived thus far with Grace, Grit and Gratitude – the grace of God and so many people connected to my days in medical school; the grit of our small team who hung in there doggedly with me despite their frustrations and exhaustion; gratitude to God for his immense mercy in keeping us safe and to our families and friends for their constant support and prayers.

Ultimately, we realise that these are unprecedented times. In The Fellowship of the Ring, Frodo says, ‘“I wish it need not have happened in my time.” “So do I,” said Gandalf, “and so do all who live to see such times. But that is not for them to decide. All we have to decide is what to do with the time that is given us.”’
But for us as Christians, the firm belief is that our times are in the Lord’s hand as it is written in Isaiah 43:1-2: ‘Do not fear, for I have redeemed you; I have summoned you by name; you are mine. When you pass through the waters, I will be with you; and when you pass through the rivers, they will not sweep over you. When you walk through the fire, you will not be burned; the flames will not set you ablaze.’
We as a small team of Christian healthcare workers in a remote and isolated corner of India can witness that this promise is true as we ourselves continue to witness to our saviour by serving the COVID afflicted in these difficult and trying circumstances.
Dr George Mathew is the medical director of Shanti Bhavan Medical Centre in Biru village in Simdega district of Jharkhand state in India. He can be reached at [email protected]
Listen to a recent webinar from Dr Mathew as he describes in more detail what it’s like to face COVID in a remote and resource-poor location.
